► IN THIS ISSUE

Loose Dentures? Don’t Panic, We Can Help!
Dentures are great technology for replacing missing teeth, but they’re also not perfect. They can be difficult to keep in, especially the lower denture. But there are ways to help you take a bite out of life better…

5 Ways Dental Veneers Can Save You A Bundle of Money and Time!
Compared with some other possible options for improving your smile, dental veneers can save you a bundle, as well as shave off the time it takes to achieve your optimum smile. Read more to find out how!

Loose Dentures? Don’t Panic, We Can Help!
Dentures are great technology for replacing missing teeth, but they’re also not perfect. They can be difficult to keep in, especially the lower denture. But there are ways to help you take a bite out of life better…

5 Ways Dental Veneers Can Save You A Bundle of Money and Time!
Compared with some other possible options for improving your smile, dental veneers can save you a bundle, as well as shave off the time it takes to achieve your optimum smile. Read more to find out how!

The Dentist Is Nothing To Be Scared About … So Why Are You Scared?
If you have been avoiding the dentist because of fear, you’re not alone. Dental phobias are among the most common, and in some cases they can be debilitating.

For Your Info: Let’s Review The Ways We Can Improve Your Smile
Here’s look at some of the modern technological advances in the field of dentistry that enable us to reshape your teeth to a more natural appearance.

The Dentist Is Nothing To Be Scared About … So Why Are You Scared?
If you have been avoiding the dentist because of fear, you’re not alone. Dental phobias are among the most common, and in some cases they can be debilitating.

How Thrush Infections Can Affect Your Dentures
Oral thrush is problem many denture wearers suffer from — but it doesn’t have to be. Here is some helpful advice on how oral thrush can be prevented.

Calcium’s A Winner For Your Smile … Here Are Some Calcium Rich Recipes!
Everyone knows, calcium protects teeth and bones, but keeping levels high enough can be a challenge. Presenting six super foods packed with calcium, and some fun recipes to help you make them taste great!

How Thrush Infections Can Affect Your Dentures
Oral thrush is problem many denture wearers suffer from — but it doesn’t have to be. Here is some helpful advice on how oral thrush can be prevented.

Can Breathing Through Your Mouth Injure Your Teeth?
Are people who breathe through their mouths more likely to have oral health issues? A recent study warns, it just might be true. If you or someone you know is a mouth breather, you should read this!

Patching Up Leukoplakia: “What’d You Call It?”
Set the scene: You bolt out of bed to get ready for your first Zoom call. In the bathroom, you manage a glance at yourself in the mirror. Opening your mouth to see how white (or yellow) your teeth are going to look on camera, you notice a thick, white/greyish patch...
► our little video
► More Good Stuff

Patching Up Leukoplakia: “What’d You Call It?”
Set the scene: You bolt out of bed to get ready for your first Zoom call. In the bathroom, you manage a glance at yourself in the mirror.
Opening your mouth to see how white (or yellow) your teeth are going to look on camera, you notice a thick, white/greyish patch just on the left side of your tongue.
If you discover a patch or lesion in your mouth, don’t panic, it’s not necessarily cancer, but it could be what the dental and medical pros call leukoplakia.
 While it’s not “The Big C”, it can possibly go that way, so it’s a great idea to understand why you have it, and how to get rid of it. Indeed, folks diagnosed with leukoplakia could possibly develop Squamous Cell Carcinoma (SCC) in the course of ten years. And white or greyish patches mixed with red speckles may be a you already have oral cancer.
While it’s not “The Big C”, it can possibly go that way, so it’s a great idea to understand why you have it, and how to get rid of it. Indeed, folks diagnosed with leukoplakia could possibly develop Squamous Cell Carcinoma (SCC) in the course of ten years. And white or greyish patches mixed with red speckles may be a you already have oral cancer.
Here’s an excellent video from the U.K.’s Oral Health Foundation…
What are the signs of leukoplakia?

There are two basic types of leukoplakia…
Non-homogenous – An essentially white or white/grey and red, unevenly shaped patch could be flat, bulges, or elevated.
Homogenous – A mostly white/grey, uniformly colored patches that are consistent throughout.
The condition may be discovered on areas of the gums, tongue, inside of cheeks or up on the palette. They could be patches or lesions that are
- Slightly raised
- Thick
- Hardened, rough
- Irregular
- Flat-textured patches
- White or gray
We decided to spare you, the gory images but here are some pics if you’re interested. These patches may not be painful but could be irritated by stimuli such as hot or cold, spices and acidic food or liquids.
What causes leukoplakia?

The potential triggers/causes include a bunch of things…
- Drinking alcohol
- Irritations from orthodontics, sharp or pointy teeth, biting the tongue, improperly fitted dentures
- HIV/AIDs
- Smoking or chewing tobacco
- Inflammation
How do you get rid of it?
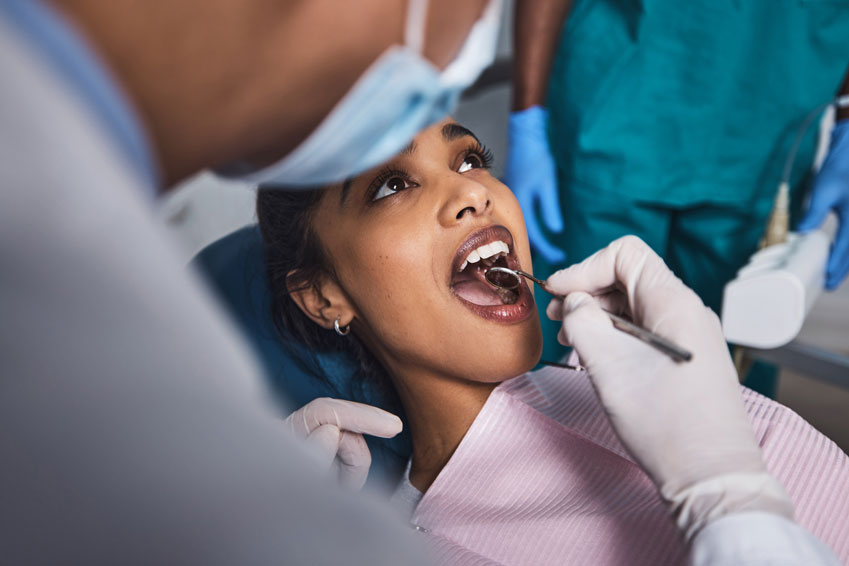
The most important way to reduce occurrences is to catch it early. Regular dental checkups will reveal its presence and hasten treatment. Equally importantly is, since it occurs because of other things, eliminating the root causes before symptoms occur is wise.
If leukoplakia doesn’t go away on its own, surgical removal is highly recommended. In addition, once you’ve got it, it is likely to come back.
Staying Healthy

As mentioned, leukoplakia is often the result of a lifestyle choice. Eating a healthy, balanced diet, regular brushing and flossing your mouth daily, refraining from smoking or chewing tobacco, reducing alcohol consumption are all recommended.
And of course, regular checkups by your dentist will help ensure thinks like leukoplakia do not go undetected – and if you see something, say something and tell your dentist.

Acid Alert! Five Facts About Your Oral Health and Snacking
Did you know? There’s a right way and a wrong way to enjoy between meal snacks. Do it the wrong way and your oral health may suffer! Check out how to snack the right way…

Straighter Teeth? Better Bite? What’s The Right Solution?
With the growing number of orthodontic treatment options available today, patients and practitioners can choose from several kinds of aligners. Which type is best for you?
So many braces, so little time! Naturally, the decision which system to use must be made by you and an experienced professional orthodontist and/or dentist. So much depends on the nature and severity of your condition, which may include…
- Overbite/deep bite
- Overjet
- Underbite
- Spacing issues
- Open bite
- Crowding issues
- Crossbite issues
- Teeth straightening
- A combination
In addition, your social needs, comfort and other factors play a role in which method you and your practitioner (hopefully, us) decide upon. Here are some general choices but note, there are many more…
Traditional Metal Braces
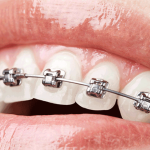 Traditional metal braces are the ones you automatically picture when someone says “braces.” Stainless steel brackets are cemented to your teeth and connected to archwires with colorful elastic rubber bands. Sturdy and reliable, these braces are capable of handling tooth and bite problems that other types of braces simply can’t.
Traditional metal braces are the ones you automatically picture when someone says “braces.” Stainless steel brackets are cemented to your teeth and connected to archwires with colorful elastic rubber bands. Sturdy and reliable, these braces are capable of handling tooth and bite problems that other types of braces simply can’t.
Self-Ligating Braces
 Much like traditional braces, self-ligating braces use brackets cemented to the teeth and an archwire. However, instead of elastics, a specialized clip is used, resulting in less friction on the tooth. Many orthodontists use the Damon System of self-ligating braces, which offers both traditional metal and clear brackets.
Much like traditional braces, self-ligating braces use brackets cemented to the teeth and an archwire. However, instead of elastics, a specialized clip is used, resulting in less friction on the tooth. Many orthodontists use the Damon System of self-ligating braces, which offers both traditional metal and clear brackets.
Ceramic Braces
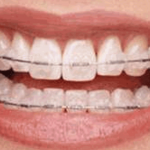 Ceramic braces use brackets made of clear ceramic instead of metal. Also known as clear braces, these braces are less noticeable than their metal counterparts. They’re also more brittle, which means they aren’t appropriate in all situations.
Ceramic braces use brackets made of clear ceramic instead of metal. Also known as clear braces, these braces are less noticeable than their metal counterparts. They’re also more brittle, which means they aren’t appropriate in all situations.
Lingual Braces
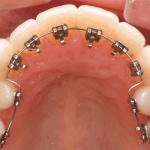 Lingual braces are traditional braces placed on the back side of the teeth. While this is appealing for cosmetic reasons, it can be more difficult for you to keep your teeth clean and for your orthodontist to make adjustments. You may also notice issues with your speech.
Lingual braces are traditional braces placed on the back side of the teeth. While this is appealing for cosmetic reasons, it can be more difficult for you to keep your teeth clean and for your orthodontist to make adjustments. You may also notice issues with your speech.
Clear Aligners
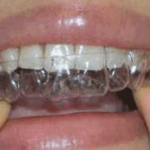 Clear aligners replace traditional brackets and arch wires with a series of computer generated acrylic trays. Each tray is worn for a few weeks at a time. Although the technology is improving, clear aligners can’t treat all orthodontic problems, and they usually require longer treatment times. But they have one definite advantage: unlike all the other types of braces, clear aligner trays are removable.
Clear aligners replace traditional brackets and arch wires with a series of computer generated acrylic trays. Each tray is worn for a few weeks at a time. Although the technology is improving, clear aligners can’t treat all orthodontic problems, and they usually require longer treatment times. But they have one definite advantage: unlike all the other types of braces, clear aligner trays are removable.
Patients aren’t restricted from sticky or hard foods and can floss easily. Practically invisible, they’re appealing if you don’t want to look like you’re wearing braces. Some brands of clear aligners, is available for teens and adults.
In recent years, mail order clear braces have become more popular as a convenient, lower-cost solution, but it is acknowledged that proper measurement and treatment of crooked teeth require careful monitoring by an experienced professional. So we do not recommend them.
Ask Your Dentist, Make A Choice – Together!
Finding the best type of braces for you or your child involves considering your orthodontic needs and your preferences regarding appearance. Complex orthodontic problems may require traditional metal or self-ligating braces, but patients with simpler issues will likely have the option of selecting more discreet styles like ceramic braces or clear aligners. Speak with your dentist first.
If you are interested in improving your smile, make an appointment with us today. Together, we can determine how best to brace yourself for the future! 🙂

The Hidden Dangers of Gum Disease
If you’ve been to the dentist recently or even browsed the oral hygiene aisle at the supermarket, chances are you’ve heard of gum disease – and you know it’s something you don’t want in your mouth.
What you may not know is just how much gum disease can put your general health at considerable risk. There are some pretty shocking links between poor oral health and the health of the rest of your body.
The Tie Between Gum Disease and Chronic Diseases
At its core, gum disease is an inflammatory condition caused by bacterial infection. Mild inflammation is called gingivitis and is usually relatively easy to reverse. Unaddressed, gingivitis can progress into full-blown advanced periodontal disease that can result in severe consequences for your teeth, gums, and overall health.
There is strong evidence to suggest that chronic gum disease can worsen other types of inflammatory diseases, including heart and lung diseases, as well as diabetes.
Because there is such an overload of bacteria present in the mouth with gum disease, it is inevitable that some of these bacteria will make its way to other parts of the body. They may settle in, on, or around organs that are already compromised due to inflammation, causing yet– more inflammation.
In conditions where inflammation already compromises the immune system and makes infection difficult to fight, such as with diabetes, the added stress of gum disease can wreak a special kind of havoc. One disease complicates the other and vice versa, making all symptoms much worse, much faster.
A Real Threat of Disability or Death
While it is unlikely that gum disease itself will kill you unless it leads to a severe abscess that goes untreated, it can contribute to life-threatening medical emergencies.
The same inflammatory response to toxins and bacteria that can exacerbate existing conditions can also create a perfect storm for a major cardiac event or stroke.
Inflammation causes arteries to narrow, which increases blood pressure, along with the risk of blood clots. It’s really only a matter of time before something goes terribly wrong.
Gum Disease and Pregnancy
Pregnant mothers who have gum disease face a substantial risk for preterm labor, which can create serious concerns for both mother and child.
Low birth weight and underdeveloped lungs are just a couple of the potential complications for the child. Inflammation in the body can also make recovery for the mother slower and more difficult.
Since pregnancy itself can often put a woman at an increased risk for developing gum disease, this is a particularly important time to keep up with regular hygiene appointments.
A Quick Fix
Perhaps the greatest tragedy in all of this is how easy it is to prevent gum disease altogether. Regular brushing, flossing, and dental check-ups can stop gum disease in its tracks and avoid all of the unnecessary complications that come with it.
If you are not sure of the best way to prevent gum disease, ask your dentist or dental hygienist to show you proper oral care techniques. It only takes a few minutes per day and can prevent a lifetime of oral and general health issues.

It's Thursday 1:44 PM — We're open!
| Monday | 8:00 AM — 5:00 PM |
| Tuesday | 8:00 AM — 5:00 PM |
| Wednesday | 7:00 AM — 4:00 PM |
| Thursday | 7:00 AM — 4:00 PM |
| Friday | Closed |
| Saturday | Closed |
| Sunday | Closed |

Chicago dentist, John J. Kelly, DDS, practices Restorative and Cosmetic Dentistry at his Chicago dental office in Edgebrook.

Can Breathing Through Your Mouth Injure Your Teeth?
A recent study demonstrates the elevated incidence of dental erosion and decay in mouth-breathers.
A study by researchers from University of Otago, Dunedin, New Zealand, published in the Journal of Oral Rehabilitation made this illuminating discovery.
OMG! How does this happen?

It’s not a secret that dry mouth, also known as xerostomia, can be an inconvenient and uncomfortable condition. But it’s still quite common. It can be caused by sleeping habits, certain medications, or even something as simple as a stuffy nose that forces you to breathe through your mouth. It can also have a real impact on your dental health in addition to being a nuisance. Here’s three reasons why a dry mouth can damage your teeth…
1. The bacteria in your mouth
Everyone’s teeth come under attack from the bacteria that live inside the mouth. These bacteria are especially active after you eat sugar or starchy, high-carb foods such as white bread. When these harmful bacteria digest sugars or starches, they create corrosive acids.
As you can imagine, having these bacteria and the acids they produce sitting on your enamel isn’t good for your teeth. The acid can eat away at the structure of your enamel. So the role saliva plays in washing away the food debris and neutralizing the acids is critical, and dry mouth gives bacteria more leeway to damage your teeth.
2. The acidic foods you consume

In addition to bacteria-produced acids, any acids in food can start to eat away at your enamel as well. That’s because acids are corrosive to teeth, pulling out the calcium, magnesium and other structural minerals that your tooth enamel uses to keep it strong. Again, saliva helps wash out acids in your mouth, but mouth-breathing prevents this from happening.
3. Remineralization complication
Saliva is your mouth’s tool to supply calcium, magnesium, and other critical substances to the outside of your enamel to help replace any minerals that leach out due to the contact from acid.
With dry mouth, you may not have enough saliva to provide the minerals that your teeth need for self-repair. In this situation, your teeth will gradually become weaker and more susceptible to cavities.
How did the study go down, again?
Groups of subjects “forced” to breathe, or not breathe, through the mouth were studied. Acidity levels of saliva in the mouth were measured. The researchers discovered that, at certain times during the night, acidity levels for mouth-breathers went beyond the threshold at which erosion of tooth enamel occurs.
Researchers saw that dentists have been reporting more patients with “dry mouth”, especially during sleep or upon awakening. Dry mouth is associated with mouth-breathing.
Mouth-breathing during sleep can cause saliva to evaporate, a defense mechanism for preventing the mouth from becoming too acidic. Acidity in the mouth can lead to enamel loss through erosion (from acid without the influence of bacteria) and tooth decay, or caries (the effect of bacteria breaking down foods to produce acid).
Researchers compared pH and temperature levels in the mouths of 10 healthy subjects. Each slept with, then without, a nose clip that forced them to breathe through the mouth.
Volunteers were given a device that measures pH and temperature of the “palatal aspect of the upper central incisors”, which they wore for two sets of 48 hours.
During the time subjects wore the clip, they experienced a drop in pH to a dangerous 3.6 – the threshold is 5.5 for when tooth enamel starts to break down.
Dr. Choi, the study’s head, concluded that, as the first study of its kind, mouth-breathing has a definitive effect on acidity levels, and the probable result of advancing tooth decay.
Mouth-breathing seems innocent enough, but it should be taken seriously. If you notice that you or someone close to you is breathing through the mouth at night, it is advisable to seek a professional evaluation with a sleep-trained dentist or other practitioner.

Patching Up Leukoplakia: “What’d You Call It?”
Set the scene: You bolt out of bed to get ready for your first Zoom call. In the bathroom, you manage a glance at yourself in the mirror.
Opening your mouth to see how white (or yellow) your teeth are going to look on camera, you notice a thick, white/greyish patch just on the left side of your tongue.
If you discover a patch or lesion in your mouth, don’t panic, it’s not necessarily cancer, but it could be what the dental and medical pros call leukoplakia.
 While it’s not “The Big C”, it can possibly go that way, so it’s a great idea to understand why you have it, and how to get rid of it. Indeed, folks diagnosed with leukoplakia could possibly develop Squamous Cell Carcinoma (SCC) in the course of ten years. And white or greyish patches mixed with red speckles may be a you already have oral cancer.
While it’s not “The Big C”, it can possibly go that way, so it’s a great idea to understand why you have it, and how to get rid of it. Indeed, folks diagnosed with leukoplakia could possibly develop Squamous Cell Carcinoma (SCC) in the course of ten years. And white or greyish patches mixed with red speckles may be a you already have oral cancer.
Here’s an excellent video from the U.K.’s Oral Health Foundation…
What are the signs of leukoplakia?

There are two basic types of leukoplakia…
Non-homogenous – An essentially white or white/grey and red, unevenly shaped patch could be flat, bulges, or elevated.
Homogenous – A mostly white/grey, uniformly colored patches that are consistent throughout.
The condition may be discovered on areas of the gums, tongue, inside of cheeks or up on the palette. They could be patches or lesions that are
- Slightly raised
- Thick
- Hardened, rough
- Irregular
- Flat-textured patches
- White or gray
We decided to spare you, the gory images but here are some pics if you’re interested. These patches may not be painful but could be irritated by stimuli such as hot or cold, spices and acidic food or liquids.
What causes leukoplakia?

The potential triggers/causes include a bunch of things…
- Drinking alcohol
- Irritations from orthodontics, sharp or pointy teeth, biting the tongue, improperly fitted dentures
- HIV/AIDs
- Smoking or chewing tobacco
- Inflammation
How do you get rid of it?

The most important way to reduce occurrences is to catch it early. Regular dental checkups will reveal its presence and hasten treatment. Equally importantly is, since it occurs because of other things, eliminating the root causes before symptoms occur is wise.
If leukoplakia doesn’t go away on its own, surgical removal is highly recommended. In addition, once you’ve got it, it is likely to come back.
Staying Healthy

As mentioned, leukoplakia is often the result of a lifestyle choice. Eating a healthy, balanced diet, regular brushing and flossing your mouth daily, refraining from smoking or chewing tobacco, reducing alcohol consumption are all recommended.
And of course, regular checkups by your dentist will help ensure thinks like leukoplakia do not go undetected – and if you see something, say something and tell your dentist.

Acid Alert! Five Facts About Your Oral Health and Snacking
Did you know? There’s a right way and a wrong way to enjoy between meal snacks. Do it the wrong way and your oral health may suffer! Check out how to snack the right way…

Straighter Teeth? Better Bite? What’s The Right Solution?
With the growing number of orthodontic treatment options available today, patients and practitioners can choose from several kinds of braces. Which type is best for you?

















